It is not unusual for a woman who has undergone tubal ligation to want to become pregnant again some years later. There are many reasons (personal, family, relationship…) to want to have another child as the circumstances vary with time, and a decision which before seemed definitive now has to be reconsidered.
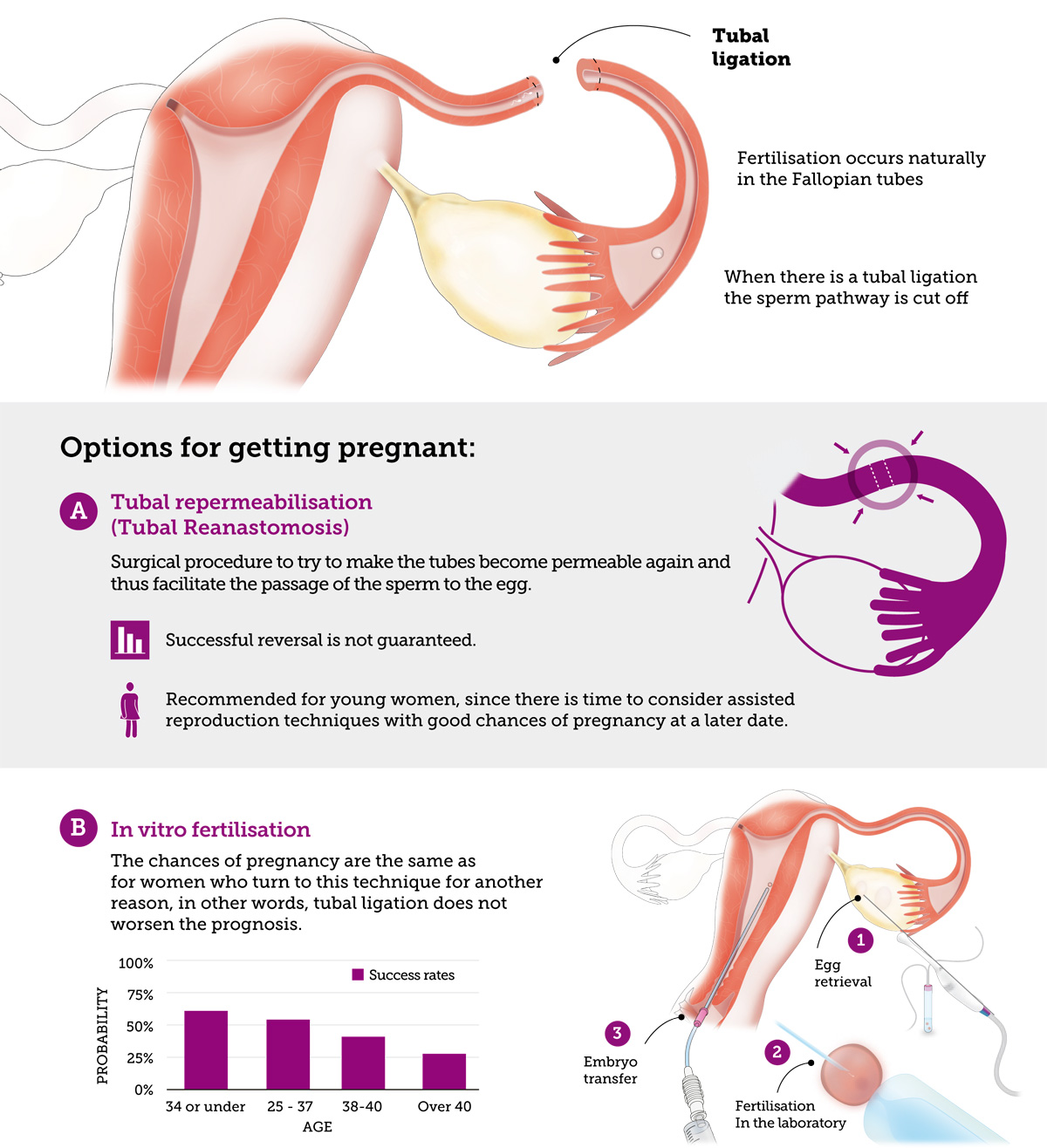
The tubal ligation technique involves surgically blocking the sperm from reaching the ampulla of the Fallopian tube and with it the fertilisation of the egg which naturally takes place in this area. Normally a segment of the tube is tied with an absorbable ligature and removed. As a result of this procedure the cut ends of the tube separate, thereby increasing the contraception effectiveness of the technique. The drawback of the treatment arises when the original function of the tubes has to be restored.
Even if attaining repermeability is technically possible, the procedure involves several disadvantages: the distance between the cut out segments and adhesion among others. Even a perfect surgical technique cannot guarantee the effectiveness of the repair as it depends on many factors (both the permeability and the motility of the tube have to be restored). However, in some cases this technique is especially recommended; for example, when very young women consider more than one pregnancy in the future.
Nowadays women who have undergone tubal ligation often choose IVF as it allows the patient to become pregnant sooner, without having to wait for the results of a surgical procedure. However, the woman’s age is a decisive factor for the successful outcome of this treatment because the chances of a pregnancy decrease with age. Therefore, once the decision has been taken it is not wise to delay it.
Tubal ligation is a definitive contraception method, which explains why women who have undertaken the operation have normally had children before (and were therefore initially fertile) which simplifies the necessary study.
- It is important to have a blood test to see if there are any hormonal alterations. The hormone basal test (FSH, LH and Estradiol) verifies the ability of the ovaries to produce eggs.
- The male partner needs a spermogram. This is a simple analysis which checks the fertilising capacity of the sperm.
- When the results of the tests are ready, the diagnosis is made and the most suitable treatment is recommended.
When the ability of the ovaries to produce eggs is confirmed and there is neither male nor endometrium pathology, in vitro fertilisation (IVF) will be recommended (Artificial Insemination cannot be undertaken when there is a dysfunction of the Fallopian tubes). IVF can be carried out in conjunction with intracytoplasmic sperm injection (ICSI) or without it.
If an endometrial polyp or myoma has been diagnosed, a hysteroscopy can be performed to confirm it. Hysteroscopy is an exploration of the interior of the uterine cavity which is normally carried out without the need of an anaesthetic. Sometimes certain pathologies can be diagnosed and even treated (for example, polyps and myomas can be removed). In this case the recommended technique is also IVF.
